Read time: 5 minutes
The American Heart Association just issued two major updates to its heart disease guidance.
Inside: two tests that could change what you know about your heart health — Lp(a) and ApoB. Neither is part of the standard lipid panel. This is big.
Heart disease is still America’s #1 killer. Up to 80% of it is preventable through lifestyle choices. In March 2026, the AHA released two major updates:
- The 2026 Dietary Guidance to Improve Cardiovascular Health (the first update since 2021)
- The 2026 Guideline on the Management of Dyslipidemia (which retires the 2018 Blood Cholesterol guideline, and yes, the name change matters)
Together, these cover both halves of the equation: what to eat, and what to test.
Don’t hold your breath waiting for your doctor to walk you through them. The gap between new guidelines and 15-minute appointments is real. Not because your doctor doesn’t care. Because the system prioritizes treatment over prevention.
So I read the guidelines. Here are 5 takeaways that should change what you ask your doctor.
1. Get Lp(a) Tested. Once. Now.
Lp(a), or lipoprotein(a), is a genetically-determined particle that raises your risk of heart attack and stroke, independent of everything else you’re doing right. It’s elevated in roughly 1 in 5 adults.
The new guidelines recommend testing it at least once in a lifetime. Most people have never had it measured because the standard lipid panel doesn’t include it.
Your Lp(a) level doesn’t change with diet or exercise. That’s not a reason to skip the test. It’s the reason to get it. If it’s elevated, your risk picture shifts, and you and your doctor can be more aggressive about every other lever you can pull.
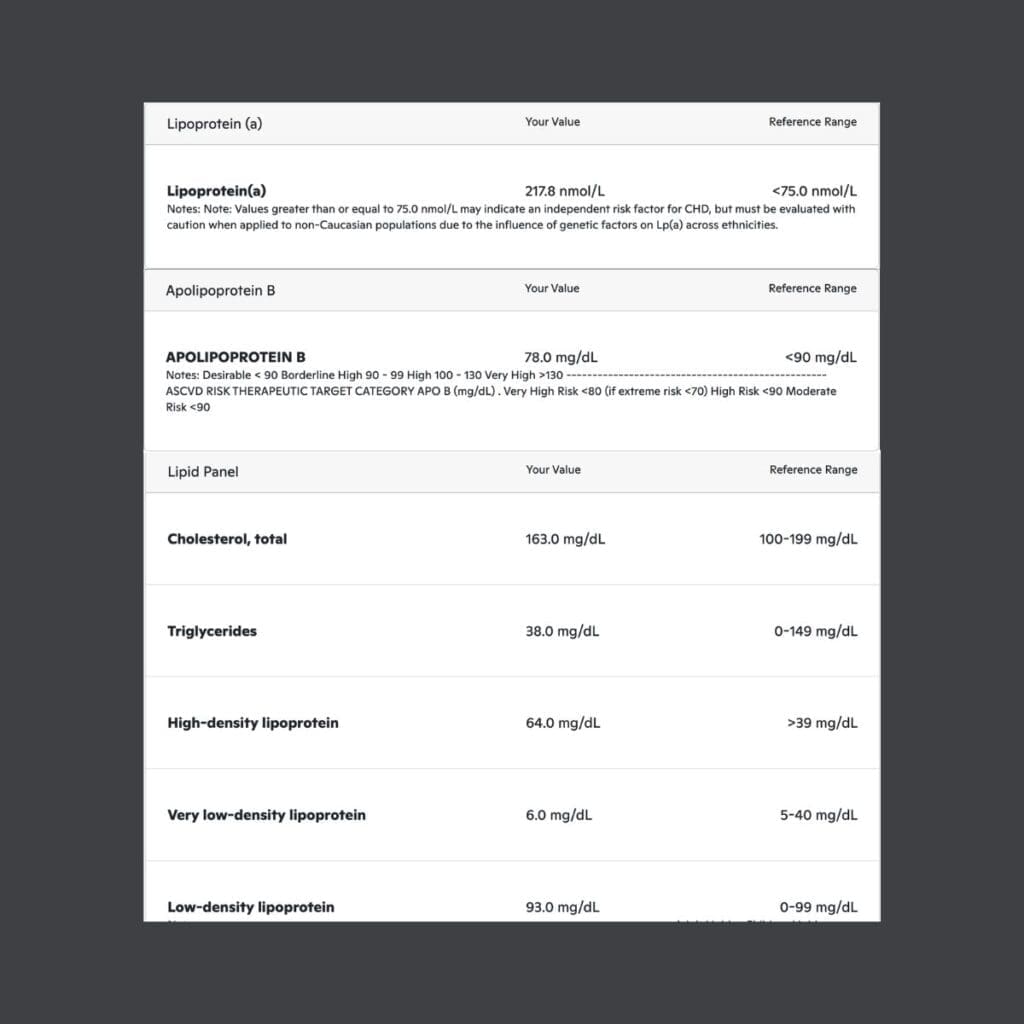
In practice: My mom’s doctor tested her Lp(a). When it came back high, I asked my doctor for the same test. Mine came back at 217.8 nmol/L — nearly 3x the threshold of 75. That’s the genetic piece in action: no amount of clean eating or training will change it. Knowing changes how aggressively you manage every other lever.
Start here: At your next physical, say: “I’d like to add Lp(a) to my lipid panel.” That’s the whole ask.
2. LDL Isn’t the Full Story. Ask About ApoB.
The 2018 guideline was “Management of Blood Cholesterol.” The 2026 version is “Management of Dyslipidemia.” That word change reflects a real shift: we’ve moved from managing a lab value to managing a condition.
The new guidelines call for selective ApoB (apolipoprotein B) testing to improve risk assessment. LDL-C measures cholesterol content. ApoB measures particle burden, which is what drives plaque formation.
Two people can have identical LDL-C numbers and very different ApoB levels. The one with more particles is at higher risk, even if both look “normal” on paper.
In practice: I asked my doctor to add ApoB to my annual labs in 2024 — heard about it on a podcast and figured better data couldn’t hurt. My most recent result (April 2026): 78 mg/dL — down from 85 last year. Standard guidelines call anything under 90 “desirable.”
For optimal prevention — and especially with elevated Lp(a) — the more aggressive target is under 80.
Start here: Request ApoB at your next physical — especially if you have family history of heart disease, diabetes, or elevated triglycerides. Same blood draw. Better data.

3. Plant Proteins Are Now the Lead
The new dietary guidance makes an explicit shift: prioritize healthy protein sources, especially plant-based options like beans, lentils, nuts, and seeds.
This is bigger than it sounds. Previous guidance treated plant and animal proteins more evenhandedly. The new language puts plants in the lead and nudges meat down the pecking order.
In practice: I’ve been whole food plant-based for 10+ years. From my April 2026 lipid panel: total cholesterol 163, LDL 93, HDL 64, triglycerides 38. The new guidance aligns with what I’ve been doing for a decade.
Start here: Swap meat for beans or lentils in one meal this week. Chili, tacos, pasta sauce, soup. Lentils and black beans slot in without drama. Bonus: a giant dose of fiber. Meat has zero.
4. Make Whole Foods the Default
The new guidance pushes for whole foods first — and limits on ultraprocessed foods, added sugars, and sodium. Most people think “ultraprocessed” means chips and soda. It’s also the lunch meat, flavored yogurt, protein bars, frozen meals, sliced bread, store-bought sauces. More than 60% of the average American diet now comes from ultraprocessed foods.
In practice: I read labels on every package, every time. The first surprise: how many “healthy” products have ingredient lists I can’t pronounce. The second: how much sodium and added sugar hide in things that don’t taste salty or sweet.
Start here: This week, read the label on every packaged food you buy. Three checks: ingredients (can you pronounce them?), added sugar, and sodium per serving.
5. Think Patterns, Not Perfection
Most of what we hear about nutrition obsesses over single nutrients (carbs! fat! protein!) or single foods (eggs are in! eggs are out!). The AHA points the opposite direction: focus on your overall eating pattern, not specific nutrients or foods.
Translation: stop chasing the latest superfood. Zoom out. Look at what’s on your plate most days.
Perfection isn’t sustainable. Patterns are. And patterns are where the compound returns live, the ones that protect your next 50 years.
Start here: Open your favorite Notes app. List what you’ve eaten the last three days. Find one repeating item (the daily yogurt, the nightly meat, the morning muffin) and swap it for a healthier version.
Not sure where to start? Reach out. Helping people troubleshoot this is what I do.
One More Thing — For Parents
Heart disease compounds. Every year of elevated cholesterol adds to lifetime risk — which is why the new guidelines push for screening to start in youth, not adulthood. I didn’t get tested until my 30s. Most pediatricians aren’t screening routinely. Ask yours.
The Bottom Line
Heart disease is the #1 killer in America. It’s also up to 80% preventable. The new guidelines tell you which levers matter most — at the doctor’s office and at the dinner table.
Pick one takeaway this week. One. Build the habit, let it compound, then layer the next.
Your heart has been working for you for decades. Time to return the favor.
Thanks for reading! Ready to bridge the gap between knowing and doing? Get weekly health insights you won’t find anywhere else. Subscribe to You Are What You Read and start turning evidence into action.
References & Additional Reading
- Lichtenstein, A. H., et al. (2026). 2026 Dietary Guidance to Improve Cardiovascular Health: A Scientific Statement From the American Heart Association. https://www.ahajournals.org/doi/10.1161/CIR.0000000000001435
- Blumenthal, R. S., et al. (2026). 2026 ACC/AHA Guideline on the Management of Dyslipidemia. https://www.ahajournals.org/doi/10.1161/CIR.0000000000001423
- Wilkinson, M. J., et al. (2024). Role of apolipoprotein B in the clinical management of cardiovascular risk in adults: An Expert Clinical Consensus from the National Lipid Association. https://www.lipidjournal.com/article/S1933-2874(24)00240-X/fulltext
- Martínez Steele, E., et al. (2016). Ultra-processed foods and added sugars in the US diet. https://pubmed.ncbi.nlm.nih.gov/26962035/
Image credit: Mike Jones
This post does not constitute medical advice. Please consult with your healthcare provider regarding your specific health needs.
Comments +